Recognizing the Signs of Chronic Sleep Problems
Sleep problems don’t always look like lying awake staring at the ceiling. They can look like sleeping 8 hours and waking up exhausted. They can look like falling asleep easily but waking at 2 or 3am and not being able to return to sleep. They can look like sleep that feels light and unrefreshing — technically adequate in duration but somehow not doing the job. They can look like a creeping fatigue that builds through the week regardless of how much time you spend in bed.
The consequences extend far beyond tiredness. Poor sleep disrupts the hormonal rhythms the body runs on. Growth hormone is released primarily during deep slow-wave sleep — chronic sleep deprivation directly suppresses this repair and recovery signal. Cortisol rhythms become dysregulated — evening cortisol stays elevated when it should be dropping, making it hard to wind down and harder to stay asleep. Testosterone production — which occurs primarily during sleep — is directly impaired by chronic sleep disruption. Insulin sensitivity worsens. Inflammatory markers rise. Cognitive performance degrades.
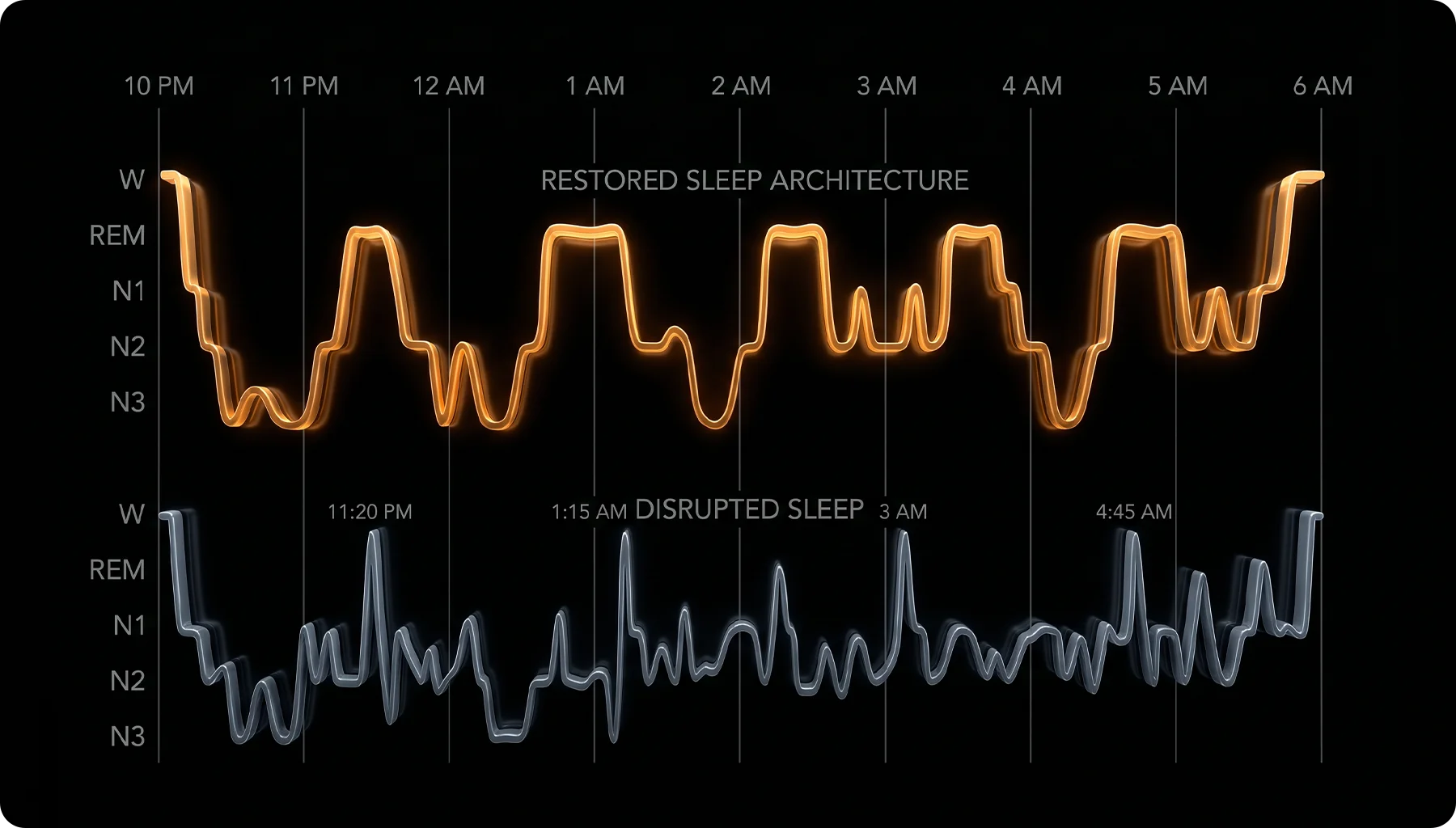
Image: Eight hours in bed isn’t the same as eight hours of sleep. Architecture is what restores you — and architecture is hormonal.
For women in perimenopause and menopause, sleep disruption is often directly tied to the hormonal transition: falling estrogen and progesterone alter sleep architecture, while hot flashes and night sweats interrupt sleep continuity at a physiological level. For men with low testosterone, sleep quality is often impaired through multiple pathways simultaneously. For anyone under chronic stress, elevated evening cortisol is one of the most common and most treatable causes of sleep-onset and sleep-maintenance insomnia.
The important takeaway: if you’ve tried sleep hygiene, avoided screens, and kept a regular schedule and you’re still sleeping badly — the problem is likely physiological, not behavioral.
Benefits of Treating Sleep Problems at Dynamis
- Restorative, Deep Sleep That Actually Recovers You
By addressing the hormonal and physiological drivers of poor sleep — rather than just sedating you through it — Dynamis protocols help restore the deep, slow-wave sleep stages that produce genuine physical and cognitive recovery overnight. - Normalized Energy Through the Day
When sleep is truly restorative, the daytime fatigue, mid-afternoon crashes, and reliance on stimulants that characterize chronic poor sleep begin to resolve — replaced by stable, sustained energy that reflects what good sleep should produce. - Improved Mood, Resilience, and Cognitive Performance
Sleep deprivation is one of the most powerful negative influences on mood and cognition. Restoring sleep quality produces improvements in emotional regulation, stress tolerance, focus, and mental clarity that patients consistently describe as transformative. - Downstream Hormonal and Metabolic Benefits
Better sleep improves testosterone production, normalizes cortisol rhythms, enhances insulin sensitivity, and supports immune function — because sleep is not just a symptom target. It’s a foundational system that everything else builds on.
What Causes Chronic Sleep Problems?
Sleep is regulated by two interacting systems: the circadian clock (the body’s internal 24-hour rhythm) and the homeostatic sleep drive (the buildup of sleep pressure over waking hours). When either system is disrupted — by hormonal imbalance, stress, light exposure, metabolic dysfunction, or substance use — the result is disrupted, non-restorative sleep.
Cortisol is one of the most important and most overlooked drivers of sleep disruption. Healthy cortisol follows a clear diurnal rhythm — high in the morning to support wakefulness and energy, declining through the day, and at its lowest in the evening to allow sleep onset. Chronic stress, adrenal dysregulation, and poor lifestyle habits can flatten this curve or invert it — with cortisol staying elevated in the evening precisely when it needs to drop.
Progesterone has a direct sedative effect through GABA-A receptor modulation. The decline of progesterone during perimenopause and menopause is a primary reason why sleep deteriorates so significantly for many women during this transition. Estrogen decline contributes through hot flashes and night sweats that interrupt sleep continuity. Low testosterone in both sexes is associated with reduced time in slow-wave sleep and increased nighttime waking.
Thyroid dysfunction — particularly hyperthyroidism or even subclinical overactive thyroid — can produce racing thoughts, elevated heart rate, and difficulty relaxing into sleep. Subclinical hypothyroidism in some patients also affects sleep architecture through fatigue-related mechanisms.

Image: The difference between waking up and waking up rested is what sleep architecture does at 3 AM — when most people are actually awake without knowing it.
At Dynamis, we assess cortisol patterns, sex hormones, thyroid function, and a full metabolic panel before making any treatment recommendations — because treating insomnia without understanding its physiological drivers is addressing the symptom and ignoring the cause.



